Substance addiction, also known as substance use disorder, is a complex condition characterized by compulsive drug or alcohol use despite harmful consequences. Several factors contribute to the development of substance addiction, including genetic predisposition, environmental influences, traumatic experiences, and co-occurring mental health disorders.
Substance addiction can involve various substances, including alcohol, opioids, stimulants, benzodiazepines, and illicit drugs like cocaine and methamphetamine. Each substance type presents unique challenges and may require tailored treatment approaches to address specific withdrawal symptoms and cravings.
Treatment for substance addiction typically involves a combination of approaches, including detoxification to safely manage withdrawal symptoms, behavioral therapies to address underlying psychological issues, medication-assisted treatment to reduce cravings and prevent relapse, and ongoing support through counseling and support groups.
What Is a Substance Abuse Addiction?
Substance use disorder (SUD), commonly known as substance abuse addiction, is a mental health condition characterized by a problematic pattern of substance use that leads to distress, impairment in daily functioning, and negative consequences. SUD encompasses a spectrum of severity, ranging from mild to severe addiction, where individuals experience an overpowering desire to use substances, increased tolerance, and withdrawal symptoms upon cessation of substance use.
Substance abuse addiction is characterized by compulsive drug seeking and use despite harmful consequences, affecting the brain and behavior. It can range from mild to severe, with addiction being the most severe form, often accompanied by dependence. Common signs include tolerance, withdrawal symptoms, cravings, and continued substance use despite negative effects.
Treatment involves a combination of therapies, medications, and support services tailored to individual needs, with early intervention and comprehensive treatment approaches improving outcomes and supporting long-term recovery.
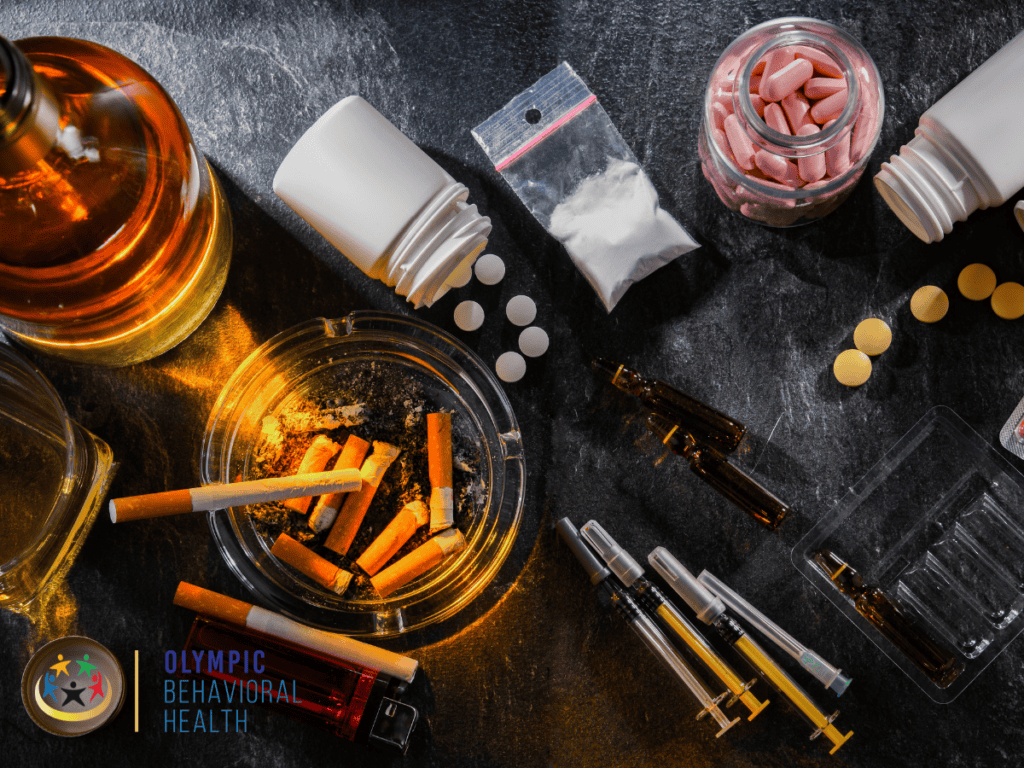
What Types of Substances Can You Be Addicted To?
Addiction can occur with a wide range of substances, each with its unique set of risks and consequences. The following list outlines some of the most common substances people can develop an addiction to.
Alcohol
Substance abuse disorder for alcohol is a condition characterized by the compulsive and harmful consumption of alcohol despite adverse consequences. It is one of the most common forms of addiction globally, affecting millions of individuals of all ages, genders, and socioeconomic backgrounds.
According to the 2022 National Survey on Drug Use and Health (NSDUH), 29.5 million people aged 12 and older in the United States had Alcohol Use Disorder (AUD) in the past year. This represents approximately 10.5% of the population in this age group.
Risks associated with alcohol addiction encompass physical health problems such as liver disease, cardiovascular issues, and neurological impairments, as well as psychological and social repercussions including depression, anxiety, isolation, and financial difficulties.
Nicotine
Nicotine substance addiction is a complex condition characterized by compulsive and habitual use of nicotine-containing products, leading to dependency and adverse effects on health. The National Institute on Drug Abuse (NIDA) reports that in 2020, approximately 8.5% of people aged 12 or older had nicotine dependence, which accounts for about 23.6 million individuals.
Common signs include persistent cravings, increased tolerance, withdrawal symptoms upon cessation, and continued use despite awareness of associated health risks. Factors such as social influences, genetic predisposition, and psychological vulnerabilities contribute to the development and perpetuation of nicotine addiction.
The risks extend beyond physical health implications to social, financial, and psychological consequences. Despite the challenges, effective treatment options are available to help individuals overcome their dependency.
Cannabis
Cannabis addiction, also known as cannabis use disorder, is characterized by increased tolerance, withdrawal symptoms, spending excessive time on cannabis-related activities, neglecting responsibilities, and continuing use despite negative consequences.
As per the National Institute of Drug Abuse (NIDA), among college-age young adults, daily cannabis use is more common than nicotine vaping, although the latter has seen a significant rise over three years. NIDA also mentions that 30% of people who use marijuana may have some degree of cannabis abuse addiction.
Risks associated with cannabis addiction include impaired cognitive function, mental health issues, respiratory problems, academic or occupational impairment, and legal consequences. Early intervention and treatment, which may include therapy, support groups, and medication, are crucial for recovery.
Food
Food addiction, characterized by compulsive eating, preoccupation with food, rapid consumption, guilt, and continuation despite negative consequences, is a prevalent issue affecting many individuals.
As per our own food addiction and eating disorder statistics research the average prevalence of food addiction globally is 20%. And only in the US, it is believed that 70 million adults are suffering from food addiction.
Risks associated with food addiction include weight gain, obesity, health complications, psychological distress, and social isolation. Seeking support and treatment, such as therapy, support groups, and nutritional counseling, is crucial for addressing the underlying emotional and psychological factors contributing to the disorder and improving overall quality of life.
Hallucinogen
Hallucinogen abuse addiction is characterized by compulsive and excessive use of hallucinogenic substances, leading to significant interference with daily functioning.
According to a study published in F1000Research in 2013 by Johansen, P.Ø., titled “Over 30 million psychedelic users in the United States,” it was estimated that there were approximately 32 million lifetime psychedelic users in the US in 2010. This study utilized data from a 2010 US population survey of 57,873 individuals aged 12 years and older to determine the lifetime prevalence of psychedelic use, including lysergic acid diethylamide (LSD), psilocybin (magic mushrooms), mescaline, and peyote.
Common signs include perception alterations, mood swings, impaired judgment, and disruptions in daily activities. Risks associated with this addiction include short-term effects like hallucinations, panic attacks, and impaired coordination, as well as long-term risks such as persistent psychosis, mood disorders, and cognitive impairment. Early recognition of hallucinogen addiction signs can facilitate timely intervention and treatment, which often involves a comprehensive approach including detoxification, psychotherapy, support groups, and pharmacotherapy.
Inhalant
Inhalant substance addiction is a serious concern characterized by the compulsive use of various substances that produce mind-altering effects when inhaled. Treatment for inhalant addiction typically involves a combination of therapy and support programs aimed at addressing the underlying issues driving the addiction and helping individuals overcome their dependence.
Data from the National Institute on Drug Abuse (NIDA) indicates that among people aged 12 or older in 2021, about 335,000 individuals had an inhalant use disorder in the past 12 months.
There are several types of inhalants commonly abused, including household products like glue, paint thinners, aerosol sprays, and cleaning fluids, as well as industrial chemicals and gasses. Inhalant abuse can lead to a range of signs and symptoms, including dizziness, euphoria, hallucinations, slurred speech, impaired coordination, and even unconsciousness. Additionally, repeated inhalant use can pose significant risks to physical and mental health, including brain damage, liver and kidney damage, heart failure, and even sudden death.
Opioid
Opioid substance addiction refers to a condition wherein individuals develop a compulsive and often uncontrollable urge to use opioids, despite the adverse consequences it may entail. Treatment for opioid addiction typically involves a multifaceted approach, incorporating medication-assisted therapies, counseling, and support groups. Medications such as methadone, buprenorphine, and naltrexone are commonly used to manage cravings and withdrawal symptoms, allowing individuals to focus on recovery and rehabilitation.
According to Dydyk, Alexander M., et al.’s 2024 publication “Mainstreaming Addiction Treatment (MAT) Act” in StatPearls, Opioid use disorder (OUD) affects over 16 million individuals globally, with more than 2.1 million cases in the United States alone. Notably, the prevalence of opioid addiction parallels that of other prevalent medical conditions such as obsessive-compulsive disorder, psoriatic arthritis, and epilepsy in the United States.
Opioid addiction is characterized by persistent cravings, tolerance, withdrawal symptoms, and preoccupation with obtaining and using the drug. Left untreated, it can lead to severe health complications, social, financial, and legal challenges, and strained relationships. Effective treatment involves a comprehensive approach, including medication-assisted therapies, behavioral therapies, counseling, and support groups, to address both the physical and psychological aspects of addiction and support individuals in their recovery journey.
Prescription Drugs
Prescription drug addiction is a complex issue often requiring therapy and treatment, with various causes and challenges faced by individuals in their recovery journey.
As per the National Center for Drug Abuse Statistics, each year, around 22.6% of prescription drug abusers, equivalent to 3.7 million people, misuse prescriptions for the first time. Around 52 million Americans, or 18.4% of the population over 12, have deliberately misused prescription drugs at least once in their lifetime. Approximately 12% of prescription drug abusers are addicted, which amounts to about 2 million individuals.
Common signs of prescription drug abuse include behavioral changes, mood swings, secretive behavior, and neglecting responsibilities. Risks include physical health complications, legal consequences, and fatal overdose. Treatment involves tailored therapies, including detoxification, behavioral therapy, support groups, and medication-assisted treatment, to address the physical and psychological aspects of addiction and promote recovery.
Stimulant
Stimulant addiction is characterized by compulsive and excessive use of stimulant drugs, leading to various adverse effects on physical and mental health.
Compton, W. M., Han, B., Blanco, C., Johnson, K., & Jones, C. M. (2018). Prevalence and Correlates of Prescription Stimulant Use, Misuse, Use Disorders, and Motivations for Misuse Among Adults in the United States. The American Journal of psychiatry indicates that approximately 6.6% of U.S. adults use prescription stimulants annually, with 5.0 million individuals misusing these medications and 0.4 million having stimulant use disorders. The motivations for misuse commonly include cognitive enhancement, and the most frequent source of misused prescription stimulants is obtaining them for free from friends or relatives. The misuse of prescription stimulants is associated with various factors such as sociodemographic characteristics, health conditions, and mental health factors.
Common signs of stimulant addiction include increased tolerance, withdrawal symptoms, neglect of responsibilities, and continued use despite negative consequences. Risks include a higher likelihood of developing mental health disorders, cardiovascular complications, and engaging in risky behaviors. Treatment involves a combination of pharmacological interventions and behavioral therapies aimed at addressing the physical and psychological aspects of addiction. With proper treatment and support, individuals can achieve recovery and lead fulfilling lives free from substance abuse.
What Are Common Signs of A Substance Abuse Addiction?
Substance abuse addiction can be challenging to detect and treat, as individuals often conceal it from loved ones. Signs to look out for include changes in behavior, neglect of responsibilities, secretive behavior, and physical symptoms. Early identification and intervention can improve recovery chances and minimize negative consequences. Seek professional or specialist assistance if you suspect someone you know is struggling with addiction.
These signs can manifest differently depending on the individual and substance being abused, such as an opioid addict exhibiting drowsiness, constipation, and needle marks versus a stimulant addict displaying increased energy, agitation, and insomnia. It’s essential to be aware of these signs, as early detection and intervention can significantly improve recovery chances and minimize potential negative consequences associated with addiction.
If you suspect your child, partner, or parent is struggling with substance abuse, seek help from a healthcare professional or addiction specialist promptly.
What Are Common Symptoms of A Substance Abuse Addiction?
Key symptoms of substance use disorder include excessive consumption, loss of control, withdrawal symptoms, tolerance, cravings, altered mood, and physical manifestations like increased heart rate and tremors.
These symptoms can vary from person to person and depend on factors such as the substance used, the duration and severity of use, and individual personality traits. Some common symptoms of substance use disorder are:
- Physical Signs:
- Sudden weight loss or gain
- Pupils that are smaller or larger than usual
- Bloodshot eyes
- Changes in appetite and sleeping patterns
- Slurred speech
- Constant fatigue
- Bloodshot eyes
- Lack of energy
- Weight loss or gain
- Psychological Signs:
- Using drugs or alcohol to soothe emotional pain like sadness, anger, or boredom
- Craving the substance
- Needing more of the substance to achieve the same effect
- Experiencing withdrawal symptoms when not using the substance
- Behavioral Signs:
- Spending a large portion of time finding, using, or recovering from the substance
- Being unable to meet obligations at home, work, or school due to substance use
- Recurring thoughts of quitting but not managing to quit successfully
- Giving up or cutting back on social or recreational activities due to substance use

What Are Examples of Substance Addiction?
Board examples of a person that has an addiction to alcohol or any other commonly used drug, so that the reader can use it to self-reflect or can use it to check if their loved one has a substance abuse addiction. Also, it would be good to mention something where it’s just a regular use which is not dangerous or addictive behavior, like a child that starts drinking with their friends but only does it irregularly.
A person with an alcohol addiction may find themselves constantly preoccupied with thoughts of drinking and obtaining alcohol. They may drink far more than intended, despite attempts to cut back or quit. Drinking takes priority over other responsibilities like work, family, or social commitments. Relationships suffer and work or school performance declines. The individual may continue drinking despite negative consequences like legal issues, health problems, or financial strain. When not drinking, they experience withdrawal symptoms like nausea, shakiness, or anxiety. Their tolerance increases over time, requiring more alcohol to achieve the desired effects.
Now compare that with this social/Non-Addictive use:
A college student enjoying a few drinks with friends on weekends would not necessarily indicate addiction or problematic use. As long as the drinking doesn’t lead to personal, academic, or legal issues, this social use may not be a cause for concern. However, it’s still important to monitor for any escalation, as addiction can develop gradually.
Watching for warning signs like loss of control over use, prioritizing the substance, relationship/occupational problems, high tolerance, and withdrawal can help identify addiction in yourself or a loved one. Any addictive behavior should be addressed promptly, but casual or infrequent use may not represent a substance use disorder. Consulting a professional for an assessment is advisable.
What Causes an Addiction?
Addiction can result from a complex interplay of genetic, psychological, and environmental factors. From genetic predispositions to social influences and mental health conditions, understanding the multi-faceted causes of addiction is vital for developing effective strategies for prevention and treatment.
Here are the causes of addiction in detail:
- Genetic predisposition: Certain individuals may have a genetic predisposition to addiction, making them more susceptible to developing substance use disorders.
- Biological factors: Biological changes in the brain, such as alterations in neurotransmitter levels, can contribute to addictive behaviors and substance dependence.
- Brain’s response to substances: Drugs and alcohol can affect the brain’s reward system, leading to the release of dopamine and reinforcing addictive behaviors.
- Early childhood trauma and abuse: Experiencing trauma or abuse during childhood can increase the risk of developing addiction later in life as a way to cope with unresolved emotional pain.
- Social influences and environment: Peer pressure, societal norms, and exposure to environments that promote substance use can influence the likelihood of developing addiction.
What Are the Risks of Having a Substance Abuse Addiction?
Effects on the Mental Health
Substance abuse addiction can contribute to the development of various mental illnesses, such as anxiety, depression, and impulse-control disorders, due to shared risk factors and brain region involvement. Genetic factors, environmental influences, and brain circuit alterations play significant roles in this interplay. Comprehensive treatment approaches are essential to address both addiction and mental health issues, with initiatives like national surveys, awareness programs, and helplines working towards prevention, education, and support.
Effects on the Body
Drug overdose resulting from substance abuse addiction can have severe physical and mental effects on the body. These effects include seizures, stroke, mental confusion, brain damage, lung disease, memory problems, attention deficits, and impaired decision-making. Additionally, substance abuse can lead to global effects on the body such as breast development in men and increased body temperature, which can further exacerbate health issues.
It’s crucial to understand that substance use disorders are treatable conditions, and seeking professional help is essential to address both the immediate and long-term effects of drug addiction. Through individualized, evidence-based treatment programs, individuals can receive the support and resources needed to overcome addiction and improve their overall health and well-being.
Effects on Personal Life
Substance abuse addiction significantly impacts personal life, extending to family dynamics, social interactions, emotional well-being, and educational and career pursuits. Family members often experience disruptions in attachment, communication, and routines, leading to emotional chaos, conflict, and financial strain. Moreover, children in such environments may become “parentified,” taking on responsibilities beyond their developmental stage, while parents may enable addictive behaviors, perpetuating the cycle.
Socially, substance abuse can lead to isolation, strained relationships, and legal issues, affecting both individuals and society at large. These effects underscore the importance of comprehensive interventions addressing family dynamics, social support, and individual recovery to mitigate the pervasive impact of substance abuse addiction.
What are Treatment Options for a Substance Abuse Addiction?
Our Substance abuse treatment encompasses a range of interventions aimed at helping individuals recover from drug and alcohol addiction. These treatments are tailored to each person’s needs and may include detoxification, intensive inpatient services, outpatient care, therapy, and ongoing support. With successful treatment and management, recovery is possible, although it may require time and a combination of treatment supports to achieve lasting sobriety.
| Treatment Name | Description |
| Detoxification | The process of safely managing acute intoxication and withdrawal symptoms while removing substances of abuse from the body. It is often the first step in addiction treatment. |
| Inpatient or Residential Treatment | Intensive treatment is provided in a residential or hospital setting, offering a highly structured and supportive environment for those with severe addiction. |
| Outpatient Treatment | Treatment that does not require overnight stays, allows individuals to live at home and attend treatment sessions regularly. This can include individual or group counseling, medication management, and other services. |
| Medication-Assisted Treatment (MAT) | The use of medications like methadone, buprenorphine, or naltrexone, combined with counseling and behavioral therapies, to treat opioid or alcohol addiction. |
| Cognitive-behavioral therapy (CBT) | A form of psychotherapy that helps individuals identify and change negative thought patterns and behaviors related to substance abuse. |
| Contingency Management | A type of behavioral therapy that uses positive reinforcement, such as vouchers or rewards, to encourage abstinence and attendance in treatment programs. |
| 12-Step Programs | Peer support groups like Alcoholics Anonymous (AA) or Narcotics Anonymous (NA), based on the 12-step model of recovery, which emphasize abstinence and personal growth. |
| Family Therapy | Counseling that involves family members to improve communication, resolve conflicts, and provide support for the person in recovery. |
| Dual Diagnosis Treatment | Integrated treatment for individuals with both a substance use disorder and a co-occurring mental health condition, like depression or anxiety. |
| Aftercare and Relapse Prevention | Ongoing support and strategies to help individuals maintain sobriety and prevent relapse after completing an initial treatment program. |
These rehab options cater to different levels of addiction severity and individual needs, to help people achieve and maintain sobriety.

Share This Post



